Tests and procedures
Different procedures and tests are used to monitor and manage your condition when you have PSC. Check out 'Your Medical Care' for details of when they might be considered.
There is no single blood test to diagnose PSC or measure its progression
However, liver blood tests are an important and regular part of the management of PSC. The tests give an indication of how well your liver is functioning and the kind of damage happening in your liver and bile ducts 52,58.
They are conducted every 6-12 months, or more frequently depending on your condition.
Your blood tests are usually carried out at your hospital or GP’s surgery. PSC Support recommends that you ask for a copy of each blood test result, so you have a complete picture of your blood history over time. Unfortunately, not all hospitals and GPs can access each other’s results, so it helps if you can track the complete picture. This way you can see straight away if your results are stable, and they are very useful to take on hospital visits to show your consultant.
Track your results
The PSC Support App allows you to track your blood test results and download reports.
PSC Support also has a downloadable liver blood test Tracker that produces a graph, thanks to member, Kevin McCabe.
Download liver blood test tracker (Excel)
What’s important about liver blood tests in PSC?
Your doctor is interested in how consistent your blood tests are over time and will look for trends. If they are stable, then your doctor will not be concerned.
Your doctor will look at the pattern of injury to identify the prominent process involved as the test results do not necessarily show the severity of injury. For example, the hepatocytes (liver cells) that are injured cause liver enzymes to leak out into the blood, and a high ALT result may reflect a young healthy person with a liver injury (with liver cells causing a lot of ALT to leak out). On the other hand, a person with cirrhosis may have a low ALT, because there are fewer liver cells left leaking out ALT.
Some people have blood tests that are completely out of the normal range for years, yet they feel well and don’t have any problems. Other patients have blood tests that are not as bad, yet suddenly develop symptoms. Therefore, it is important to understand past liver blood test trends to help predict what will happen in the future.
Liver blood tests explained
Liver blood tests are sometimes referred to liver function tests (LFTs) but this is somewhat outdated because the blood gives more information than just liver function.
- Alkaline Phosphatase (ALP) - high levels can indicate damage or obstruction in the bile ducts. It can also be raised in non-liver issues such as: the presence of bone disease, fractures, heart problems, pregnancy. It is also common for young people to have raised ALP levels.
- Gamma-Glutamyl Transferase (GGT) - high levels of GGT may indicate liver damage. This is used to understand whether the elevated ALP relates to liver or non-liver issues. Because ALP is not a reliable marker for PSC in children, GGT is considered to be a more specific marker of bile duct injury in children, and children tend to have much higher levels of GGT, AST and ALT than in adults 130.
- Alanine Aminotransferase (ALT) and Aspartate Aminotransferase (AST) - measure damage in your liver cells (hepatocytes).
- Bilirubin - informs about how your liver is functioning. It is cleared by the liver and high levels can indicate a blockage of the bile ducts or liver damage. It means that your liver is no longer breaking down waste properly and can cause jaundice (where your skin and eyes appear yellow).
- Albumin - informs about liver function. It is a protein that is only produced in the liver. Low levels can indicate a liver which is not functioning properly.
- INR (international normalised ratio) - informs about how the liver is functioning by showing how quickly the blood clots. A higher INR can also reflect vitamin K deficiency.
Enhanced Liver Fibrosis (ELF) Test
The ELF test is a blood test that measures three parameters involved in the process of developing fibrosis. A score is then calculated to give an estimate of the severity of fibrosis in your liver and can be used to make an estimate about what might happen to you 42,43.
Resources
There is more detailed information about liver blood tests in the 2017 British Society of Gastroenterology Guidelines on the Management of Abnormal Liver Blood Tests (co-authored by PSC Support):
Everything you need to know about having a colonoscopy, including managing the bowel prep and pre-colonoscopy foods.
Measuring bone density
Bone density is measured using a DXA (dual energy X-ray absorptiometry) scan.
You will be asked to lie on a bed and stay still while the scanner, a kind of X-ray machine, moves over the different parts of your body being scanned. The procedure is painless and will take approximately 15 minutes.
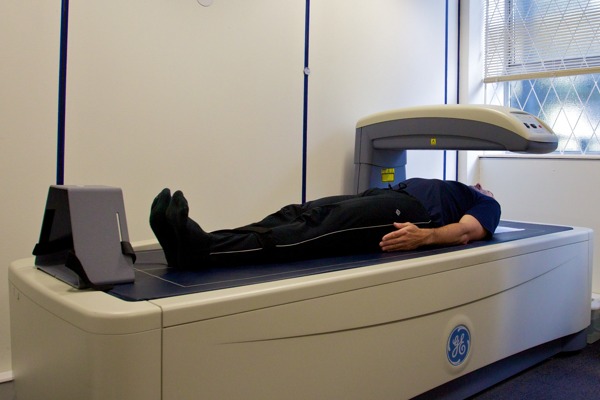
Photo credit: Nick Smith photography - ALSPAC web site, CC BY-SA 3.0
ERCP is short for Endoscopic Retrograde CholangioPancreatogram
Diagnostic ERCP is when X-ray contrast dye is injected into the bile duct, the pancreatic duct, or both and X-rays are taken to get pictures of these ducts. Because the ERCP is an invasive procedure, it is usually only carried out if there will also be some therapeutic value to the patient.
ERCP allows examination of the tubes that drain the liver and pancreas. It is mainly used to study these areas and then conduct a therapeutic procedure in narrowed or obstructed tubes. It may be used to treat jaundice, episodes of cholangitis or ascending cholangitis, significant increases in your bilirubin, to remove stones, insert stents and clear blockages.
ERCPs should be carried out after expert clinico-radiological assessment to justify the procedure. BSG/UK-PSC Guidelines Recommendation 12 58.
Dominant strictures
Dominant biliary strictures develop in up to 50% of patients with PSC. This is where the common bile duct narrows to less than 1.5mm or less than 1mm in a hepatic duct. Sometimes, dominant strictures can lead to complications such as jaundice, cholangitis and itch or deterioration in liver biochemistry, in which case ERCP may be performed 131. Dominant strictures can be balloon dilated at ERCP (see below).
What happens in an ERCP?
ERCP is usually carried out under sedation: this means you will be relaxed but not completely asleep. You may be able to go home when you have recovered from the procedure but some people remain in hospital overnight to be monitored.
- Patients receive a local anaesthetic that is gargled or sprayed on the back of the throat; this anaesthetic numbs the throat.
- A needle is inserted into a vein in the arm if sedatives are to be given. You will be monitored throughout the procedure.
- During an ERCP, you will lie on your back or side on an X-ray table.
- The doctor inserts an endoscope (thin flexible tube) through the mouth, down the oesophagus, through the stomach, and into the duodenum. Video is transmitted from a small camera attached to the endoscope to a computer screen. Air is pumped through the endoscope to inflate the stomach and duodenum, making them easier for the doctor to examine.
- During the ERCP, biliary stenting or balloon dilatation can take place, which has been shown to improve the liver biochemistry/symptoms 131. Balloon dilatation should be the initial treatment of choice for dominant strictures in patients with PSC, as they are associated with less complications that stent dilatation 132.
Read a patient experience of ERCP
Stents
When a narrowing of the bile ducts is discovered, a short tube (a stent) can be inserted. This will open the bile duct and allow the bile to drain. The tubes do not last forever and over time can become blocked, at which point the procedure may be repeated.
Strictures (narrowing) within the liver may not be appropriate for stenting because they are not easily accessible.
Balloon dilatation
Balloon dilation is another option if a narrowing of the bile ducts is discovered. A tiny tube with a balloon on the end is inserted into the bile duct. At the narrowing (stricture), the balloon is inflated and deflated several times to expand the duct so the bile can flow through once more. Because the bile ducts can sometimes quickly return to their narrowed state, sometimes a stent is placed at the stricture point.
When the doctor has located the correct position, dye is injected into the bile ducts, allowing them to be seen on X-rays. X-rays are then taken to show the ducts and to look for narrowed areas or blockages.
After the ERCP
Following the procedure, you will be monitored to see when it is appropriate for you to go home, and you must have someone with you for 24 hours. Some patients experience abdominal discomfort or bloating because of the air that was pumped into them. In some cases, patients may suffer attacks of pancreatitis or cholangitis. If there are any complications, you will remain in hospital following the procedure.
Complications following ERCP
Cholangitis flares and pancreatitis can occur following ERCP, so current guidelines recommend antibiotics are given prior to the procedure taking place as a precautionary measure 67 and for 5-7 days after the procedure. See BSG/UK-PSC Guidelines Recommendation 10 58.
People who have an ERCP are likely to have another one in the future. It is important that you discuss this procedure carefully with your consultant and understand the complications that may arise. Most people suffer little discomfort and complications following this procedure.
Videos
ERCP in PSC Dr Deepak Joshi
This video was taken from Dr Deepak Joshi's presentation to primary sclerosing cholangitis patients at our London 2019 Information Day
This video covers: The basic anatomy, ERCP - what, when, why, how?, Pre, per- and post- ERCP care
The Role of ERCP in PSC - Dr Roger Chapman
Dr Roger Chapman talks to patients at our 2016 Oxford Information Day about ERCPs, covering what strictures are, MRCPs, ERCPs, risks, what ERCPs are used to do including stents and balloon dilatation.
Fibroscan uses transient elastography, which is a technique similar to ultrasound, that measures the stiffness of your liver.
It is a non-invasive test and the level of stiffness is thought to represent the degree of scarring in the liver. The more stiffness there is, the higher the score, indicating a higher degree of fibrosis (scarring).
In PSC, the Fibroscan score is more useful if the score is very low (under 7) or high (over 40). Scores in between can be difficult to interpret. Liver scarring and fibrosis is not the only reason for a high Fibroscan score. It can be high if you have eaten (as that increases the blood flow to the liver) or if there is blockage of the bile ducts.
What happens during a Fibroscan?
You will be asked not to eat for two hours before your Fibroscan.
- When you arrive you will be asked to lie on the bed with your right arm behind your head. You will uncover the side of your body.
- The scanner places a probe on your skin, between two ribs on your right side, and the test will begin. You will feel a pulse as though someone is tapping or thumping you on your skin.
A Fibroscan takes only a few minutes.
Photo credit: Slaurent73 - CC BY-SA 4.0
A gastroscopy is an investigation of the oesophagus, stomach and duodenum
What happens during a gastroscopy?
- A thin tube is passed through the mouth into the areas to be investigated and a video is transmitted to a screen which the doctor can see.
- You will be given a choice about whether or not to have sedation for this procedure. Many people have a more positive memory of this procedure if they take the maximum amount of sedation on offer, although some have no sedation and have equally positive reports.
- You may receive a local anaesthetic to numb the throat that can be gargled or sprayed. It is often banana flavour! Sedation may be administered through a vein in the arm or hand. This helps you stay relaxed, comfortable and drowsy but it is not the same as a general anaesthetic.
- Air is pumped through the endoscope to inflate the stomach and duodenum, making them easier to see.
- Special tools are slid through the endoscope which allow the doctor to take some small samples of tissue for examination (biopsies). If you have varices, these may be banded at the endoscopy.
- If you have opted for sedation, you will be monitored for about an hour after the procedure while it wears off. You may be aware of the air that has been pumped in, and have a sore throat from the tube for a couple of days.
ERCP is short for Endoscopic Retrograde CholangioPancreatogram
Diagnostic ERCP is when X-ray contrast dye is injected into the bile duct, the pancreatic duct, or both and X-rays are taken to get pictures of these ducts. Because the ERCP is an invasive procedure, it is usually only carried out if there will also be some therapeutic value to the patient.
ERCP allows examination of the tubes that drain the liver and pancreas. It is mainly used to study these areas and then conduct a therapeutic procedure in narrowed or obstructed tubes. It may be used to treat jaundice, episodes of cholangitis or ascending cholangitis, significant increases in your bilirubin, to remove stones, insert stents and clear blockages.
ERCPs should be carried out after expert clinico-radiological assessment to justify the procedure. BSG/UK-PSC Guidelines Recommendation 12 58.
Dominant strictures
Dominant biliary strictures develop in up to 50% of patients with PSC. This is where the common bile duct narrows to less than 1.5mm or less than 1mm in a hepatic duct. Sometimes, dominant strictures can lead to complications such as jaundice, cholangitis and itch or deterioration in liver biochemistry, in which case ERCP may be performed 131. Dominant strictures can be balloon dilated at ERCP (see below).
What happens in an ERCP?
ERCP is usually carried out under sedation: this means you will be relaxed but not completely asleep. You may be able to go home when you have recovered from the procedure but some people remain in hospital overnight to be monitored.
- Patients receive a local anaesthetic that is gargled or sprayed on the back of the throat; this anaesthetic numbs the throat.
- A needle is inserted into a vein in the arm if sedatives are to be given. You will be monitored throughout the procedure.
- During an ERCP, you will lie on your back or side on an X-ray table.
- The doctor inserts an endoscope (thin flexible tube) through the mouth, down the oesophagus, through the stomach, and into the duodenum. Video is transmitted from a small camera attached to the endoscope to a computer screen. Air is pumped through the endoscope to inflate the stomach and duodenum, making them easier for the doctor to examine.
- During the ERCP, biliary stenting or balloon dilatation can take place, which has been shown to improve the liver biochemistry/symptoms 131. Balloon dilatation should be the initial treatment of choice for dominant strictures in patients with PSC, as they are associated with less complications that stent dilatation 132.
Read a patient experience of ERCP
Stents
When a narrowing of the bile ducts is discovered, a short tube (a stent) can be inserted. This will open the bile duct and allow the bile to drain. The tubes do not last forever and over time can become blocked, at which point the procedure may be repeated.
Strictures (narrowing) within the liver may not be appropriate for stenting because they are not easily accessible.
Balloon dilatation
Balloon dilation is another option if a narrowing of the bile ducts is discovered. A tiny tube with a balloon on the end is inserted into the bile duct. At the narrowing (stricture), the balloon is inflated and deflated several times to expand the duct so the bile can flow through once more. Because the bile ducts can sometimes quickly return to their narrowed state, sometimes a stent is placed at the stricture point.
When the doctor has located the correct position, dye is injected into the bile ducts, allowing them to be seen on X-rays. X-rays are then taken to show the ducts and to look for narrowed areas or blockages.
After the ERCP
Following the procedure, you will be monitored to see when it is appropriate for you to go home, and you must have someone with you for 24 hours. Some patients experience abdominal discomfort or bloating because of the air that was pumped into them. In some cases, patients may suffer attacks of pancreatitis or cholangitis. If there are any complications, you will remain in hospital following the procedure.
Complications following ERCP
Cholangitis flares and pancreatitis can occur following ERCP, so current guidelines recommend antibiotics are given prior to the procedure taking place as a precautionary measure 67 and for 5-7 days after the procedure. See BSG/UK-PSC Guidelines Recommendation 10 58.
People who have an ERCP are likely to have another one in the future. It is important that you discuss this procedure carefully with your consultant and understand the complications that may arise. Most people suffer little discomfort and complications following this procedure.
Videos
ERCP in PSC Dr Deepak Joshi
This video was taken from Dr Deepak Joshi's presentation to primary sclerosing cholangitis patients at our London 2019 Information Day
This video covers: The basic anatomy, ERCP - what, when, why, how?, Pre, per- and post- ERCP care
The Role of ERCP in PSC - Dr Roger Chapman
Dr Roger Chapman talks to patients at our 2016 Oxford Information Day about ERCPs, covering what strictures are, MRCPs, ERCPs, risks, what ERCPs are used to do including stents and balloon dilatation.
Fibroscan uses transient elastography, which is a technique similar to ultrasound, that measures the stiffness of your liver.
It is a non-invasive test and the level of stiffness is thought to represent the degree of scarring in the liver. The more stiffness there is, the higher the score, indicating a higher degree of fibrosis (scarring).
In PSC, the Fibroscan score is more useful if the score is very low (under 7) or high (over 40). Scores in between can be difficult to interpret. Liver scarring and fibrosis is not the only reason for a high Fibroscan score. It can be high if you have eaten (as that increases the blood flow to the liver) or if there is blockage of the bile ducts.
What happens during a Fibroscan?
You will be asked not to eat for two hours before your Fibroscan.
- When you arrive you will be asked to lie on the bed with your right arm behind your head. You will uncover the side of your body.
- The scanner places a probe on your skin, between two ribs on your right side, and the test will begin. You will feel a pulse as though someone is tapping or thumping you on your skin.
A Fibroscan takes only a few minutes.

Photo credit: Slaurent73 - CC BY-SA 4.0
A gastroscopy is an investigation of the oesophagus, stomach and duodenum
What happens during a gastroscopy?
- A thin tube is passed through the mouth into the areas to be investigated and a video is transmitted to a screen which the doctor can see.
- You will be given a choice about whether or not to have sedation for this procedure. Many people have a more positive memory of this procedure if they take the maximum amount of sedation on offer, although some have no sedation and have equally positive reports.
- You may receive a local anaesthetic to numb the throat that can be gargled or sprayed. It is often banana flavour! Sedation may be administered through a vein in the arm or hand. This helps you stay relaxed, comfortable and drowsy but it is not the same as a general anaesthetic.
- Air is pumped through the endoscope to inflate the stomach and duodenum, making them easier to see.
- Special tools are slid through the endoscope which allow the doctor to take some small samples of tissue for examination (biopsies). If you have varices, these may be banded at the endoscopy.
- If you have opted for sedation, you will be monitored for about an hour after the procedure while it wears off. You may be aware of the air that has been pumped in, and have a sore throat from the tube for a couple of days.
A liver biopsy is an invasive procedure that takes very small samples of liver tissue for investigation (about 1/50,000th of your liver).
It is used to look at damage to the liver, but not used for diagnosis of PSC unless small duct PSC or another autoimmune liver disease is suspected. Because of the information it can give, and the lack of non-invasive tests to measure progression in PSC, liver biopsy is a valuable test in PSC research studies and clinical trials.
What happens during a biopsy?
You will be asked not to eat anything for at least 4 to 6 hours before you have your biopsy.
- For the procedure, you will be asked to lie on your back and a small area of your RUQ will be numbed. A biopsy needle is then inserted through your abdominal wall. Ultrasound is used to guide the needle to the correct place.
- For some biopsies, the needle is inserted through your neck (transjugular biopsy) and the needle is guided by x-ray.
- You will often be told to hold your breath while the biopsies are taken. You may be aware of a feeling like pinching deep inside you when the biopsies are taken.
- Once the biopsy needle is removed pressure is applied to stop any bleeding. The samples are then sent off to the laboratory for examination.
- After the biopsy, you have to lie still for four to six hours. You will be monitored during this time. In most cases, you will be seen as a day case. Occasionally you will be kept overnight.
Does a liver biopsy hurt?
You may experience some discomfort or pain. If you feel nervous about having a biopsy, talk to your doctor well in advance of the procedure so that sedation can be arranged. Women sometimes find that they are unable to wear a bra immediately afterwards but might find a crop type top useful for support.
MRI scan
MRCP (Magnetic resonance cholangiopancreatography) is a type of MRI scan:
- ‘cholang’ refers to the bile ducts
- ‘pancreato’ refers to the pancreas
- ‘gram’ refers to a type of X-ray/imaging
So in other words, it is a long-winded term for MRI imaging of your bile ducts and pancreas.
Magnetic resonance imaging (MRI) uses a strong magnetic field and radio waves to produce images of the inside of your body. MRI scanning is one of the safest imaging techniques available; it is non-invasive, painless and does not contain any ionising radiation.
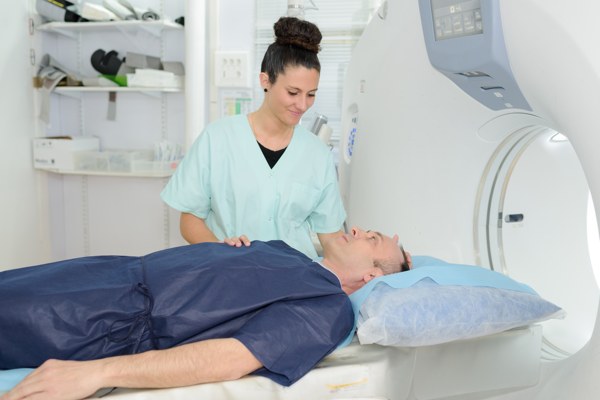
Gold standard for PSC diagnosis
MRCP is used to look at the biliary tree and is considered the ‘gold standard’ in diagnosing PSC and monitoring changes in the bile ducts over time 129. This is an important test in PSC, but can be difficult to interpret, especially if the picture is blurry because of any movement during the scan. Experts from the international PSC study group (IPSCSG) recommend patients should be assessed in experienced centres which include the performance and interpretation of MRI 129. They also recommend that patients unable to travel to specialty centres should have their MRI/MRCP images and clinical course reviewed by multidisciplinary teams with experience in PSC diagnosis and treatment 129.
It is important to wait to speak with your PSC doctor following an MRCP, because this test alone does not give a full picture of what’s going on. Your doctor looks at the MRCP in combination with your medical history, blood and other test results.
There is no agreed frequency for MRCPs in the management of PSC but you should have an MRCP if you have new or changing symptoms or evolving abnormalities in laboratory investigations: BSG/UK-PSC Guidelines Recommendation 11 58,
What happens during an MRCP scan?
You will usually be asked to restrict eating and drinking before your MRI scan. Please follow any instructions you are given carefully.
- Before your scan, you will be asked to remove all metal objects. This includes earrings and piercings, zips, belts, glasses and underwired bras. MRCP cannot be performed if you have had a cardiac pacemaker inserted, although there are now new MRI compatible devices now.
- You will enter the scanning room and you will see a large tube-shaped machine. This is the scanner. You will be asked to lie on the bed part, and you will be positioned correctly and secured in place. Make sure you ARE comfortable, because you have to lie in the same position for some time. Some people find it helpful to have a pillow placed under their feet.
- You will sometimes be given an injection (called contrast) just before you are moved into the scanner. If this is the case, you may need to lie on your back with your arms behind your head. Again, make sure you are comfortable. You might need a cushion or support under your elbows. An injection will only be given if the doctors want an MRI of your liver in addition to an MRCP.
- Once you are ready, the staff will place a communication buzzer in your hand and tell you how to use it.
- They then move the bed into the MRI scanner, which is like a short tunnel. Your head will be inside the MRI scanner and this can make some people feel claustrophobic. If you think this is likely to happen it is a good idea to close your eyes as you enter the scanner and keep them closed throughout.
- The staff then leave the room and communicate with you through speakers and a microphone in the scanner. You will be able to speak to and hear the staff at all times.
You can use the communication buzzer at any time to signal to the staff that you want to be removed. The scanner is very noisy but is completely painless.
Part of the scan involves lying very still. At some points, you are asked to hold your breath for a little while so they can get perfect images.
An MRI scan takes around 30 minutes. Some hospitals play music for your while you are in the scanner.
Ultrasound uses sound waves to generate an image for assessment, diagnosis and monitoring of various body parts. It is the same procedure that is used in pregnant women. It is safe, non-invasive and completely painless.
What happens during an ultrasound scan?
You may be asked to fast (not eat) for up to six hours ahead of your ultrasound scan, and stop drinking water a few hours before.
You will be asked to lie down and to pull back your clothing to reveal your abdomen. Gel will be applied to your skin to allow the scanner’s probe to glide over your skin and help the sound waves to be transmitted into the body. The probe transmits images on to a screen, which you will be able to see. You won’t feel anything apart from coldness of the gel and possibly a small amount of pressure. You may be asked to change positions during the scan and to hold your breath for short intervals to allow the scanner to be positioned correctly and so the correct images can be taken.
The ultrasound scan is used to look at the shape and size of liver, gallbladder and spleen, and for any abnormalities which may require further investigation. Inflammation in the bile ducts can occasionally be seen although this is not the purpose of the ultrasound scan in PSC.
How long do ultrasound scans take?
Ultrasound scans normally take about 20 minutes.
New, more advanced ultrasound scans are now being developed and available in some hospitals:
- Shear Wave Elastography - a special, advanced kind of ultrasound that can measure liver (and also spleen) stiffness.
- 2D-Shear Wave Elastography - gives a more detailed assessment over a larger areas of the liver.

